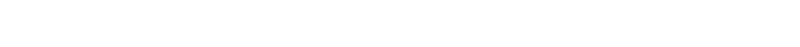As medical director of the Richmond Ambulance Authority, Dr. Joseph Ornato thinks of himself as a businessman.
“We’re in the business of saving lives,” said Ornato, who’s also the department chairman of emergency medicine at VCU Medical Center. “And time is the enemy.”
It’s Ornato’s interest in cheating time that spurred his latest project: outfitting drones with lifesaving medicine that he believes can be delivered up to five times faster by air than by ambulance.
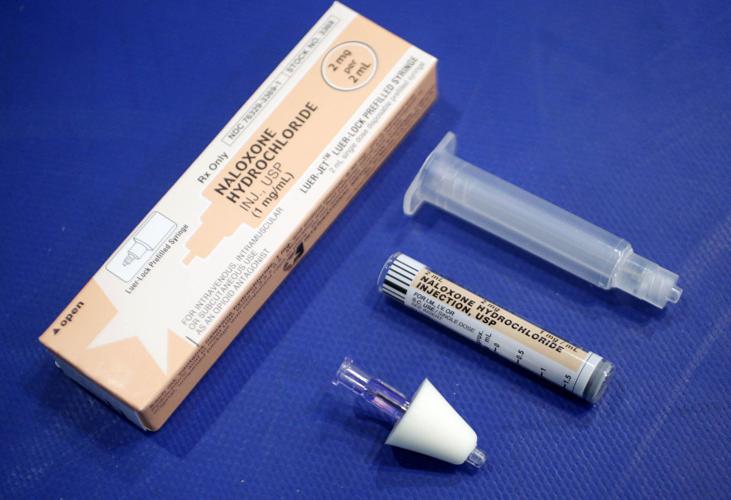
He has been working with the Virginia Commonwealth University College of Engineering for about a year and a half to pilot a program that would deliver naloxone to the scene of an opioid overdose. Legal and technological hurdles remain, but Ornato thinks he’ll have drones delivering across Richmond, at least as part of a trial, as soon as next year.
People are also reading…
Ornato envisions a 911 operator piloting a drone to the caller’s location and guiding a bystander over the phone on how to use the nasal spray, which quickly reverses the effects of an opioid overdose. By the time the ambulance arrives, ideally, the victim would already be revived.
Opioids have killed more than 9,100 people in Virginia since the state began tracking the death toll in 2007. In Richmond, the rate of overdose deaths has been double to triple the state average in each of the past five years.
Leaders in the state have recognized the importance of naloxone in saving lives, subsidizing its cost for local EMS departments, creating a standing order that allows Virginians to access it over the counter, and running training programs in which residents can receive free doses.
But many who suffer from addiction remain unaware of the programs, said Emily Westerholm, who coordinates the comprehensive harm reduction program at Health Brigade, a Richmond health services clinic geared toward low-income people. Health Brigade provides a free training program where naloxone is distributed, but many patients are surprised when they hear about it.
RAA is still regularly called to the scene of overdoses where no one has naloxone on hand. Through June, emergency personnel have administered Narcan, a brand-name version of naloxone, 420 times this year. In 2018, they used 894 doses.
Ornato knows every second is precious when emergency vehicles head to a scene to save the life of someone overdosing on the deadliest drugs in the nation.
With the help of drones, he said, a process that takes 10 minutes to get the drug to the patient could be cut to as little as two minutes.
***
Once a victim’s heart stops, Ornato said, each minute that goes by before paramedics or others can attempt to restart it equals a 10% loss in the chances of survival.
Opioid overdoses are often relatively slow, restricting a victim’s ability to breathe. But with the increasing popularity of the opioid fentanyl, which can be 50 times more potent than many forms of heroin, the body’s ability to breathe is being shut down faster.
Recent research also suggests that opioid overdoses are more linked to cardiac arrest than previously known, with an estimated 15% of out-of-hospital cases coming as a result of opioid overdoses, Ornato said.
Richmond’s EMS system is among the best in the country in terms of speed and effectiveness, with response times averaging five minutes, Ornato said. But even with an efficient system, there are many points between call and care that consume precious time — the one to three minutes, if not much longer, it takes a victim or bystander to call 911, the 30 to 60 seconds the operators require to learn details and dispatch a unit, the minute it takes emergency personnel to locate the victim and unload their gear and the final minute or so it takes EMS to establish the problem and begin care. All factors considered, it can take nine to 10 minutes for a victim to receive aid — on a good day.
If saving lives is the goal and time is the enemy, no matter how good the system is, innovation exists in spaces where you can “cheat” time, Ornato said, and he’s done it in the past by giving bystanders the ability to help.
In the ’90s, he led a study testing whether people could save more lives by using automated external defibrillators, or AEDs, when someone goes into cardiac arrest. A group trained to use the devices saw a survival rate for victims twice as high as a group trained only in CPR.
Thanks to the work of Ornato and others, the Food and Drug Administration changed the requirements for AED use, and Congress passed the Cardiac Survival Act, signed into law by President Bill Clinton in 2000, which provides for AEDs in federal buildings and protects people who use them from lawsuits.
The idea behind that study has guided Ornato’s passion: finding novel ways to save people.
“It’s really trying to figure out ways that we can empower laypeople and bystanders to — more rapidly than we can get the medical teams to them — be able to do things that are effective, or at least potentially effective, to help save a life at a stage of an emergency,” Ornato said.
Westerholm, the coordinator at Health Brigade, said any effort to expand access to naloxone is a positive. More than 80% of her clients take naloxone with them at distributions and training sessions, she said.
But when bystanders call 911, they will often say the victim is not breathing rather than use the word “overdose” to avoid legal repercussions, Westerholm said, complicating a 911 operator’s decision to send a drone and thereby limiting the potential speed of care.
Westerholm also noted communities that are skeptical of police and medical services may not be as welcoming, noting more than 50% of her participants have had naloxone administered by a friend or community member rather than officials. While that figure conveys the distrust, it also speaks to bystanders’ ability to successfully administer the antidote.
“I’m a huge supporter of the idea,” Westerholm said. “I do worry a little bit about how drones would be welcomed into particular communities.”
***
The drone proposal would not fly under current regulations, Ornato said, because commercial drone use, medical or not, has been tightly regulated. But likely changes to federal regulations and the fact that naloxone injectors weigh only a few ounces and will be easy for drones to carry give him some confidence that his project is feasible from a legal standpoint.
“It’s all feeling like the timing is, at least over this next one to three years, a lot of the elements that could potentially be showstoppers are all starting to feel like they’re coming into play,” he said.
Ornato, a licensed pilot, already has someone willing to train the 911 operators to fly drones.
Developing the drone hardware took four VCU students a year to finish. At the College of Engineering, seniors spend their final year working on capstone projects, supervised by faculty and often in conjunction with outside sponsors. Ornato came in with the idea and attracted Tamer Nadeem, an engineering professor who felt the project aligned with his research interests of wireless networks and cyberphysical systems.
Throughout the 2018-19 school year, the engineering students, under Nadeem’s supervision, worked to develop the hardware and software for the drone. The students added code and communications features to a drone, purchased by the school, that allow it to communicate with the RAA computer system and use GPS coordinates from that system to help guide the flight. The type of drones required cost about $5,000 to $10,000, Ornato said.
A second capstone team next year will refine the project further, including extending the system to support multiple drones and overcoming potential flight obstacles without restricting routes, Nadeem said. The team also needs to predict and correct any communications challenges.
“We need to add more intelligence into the [video stream] to handle if you lose connection, if you don’t have a good bandwidth,” Nadeem said. “So you need to sustain and maintain a reasonable communication back and forth. There are a lot of, still, new features. And we have to enhance the current functions that we already have.”
Keeping realistic expectations for funding and functionality, Ornato envisions the first major deployment to be three to four drones just in the city of Richmond.
“It turns out that with just three or four drones, we could have the drone land at the bystander caller’s location in a median time of 43 seconds after the dispatch,” Ornato said. “And the maximum time would be less than one minute and 20 seconds.”
“With just three or four in the city of Richmond — that’s something,” he said, before repeating his mantra. “Time is the enemy.”
***
Ornato is applying for grants to keep his project going. Any further steps will require “substantial funding,” he said. While Nadeem and the students continue to work on the drone system next year, he will be waiting on the grants, which could take up to a year.
If they’re successful, the next step would be to run a limited trial in Richmond, assuming the trial receives formal approval from VCU’s human research committee.
With funding and approval, which could all be in place in 2020 if things go well, a one-year trial of the system would likely just take place in downtown Richmond, Ornato said. He said friends and colleagues at other Virginia universities are interested in conducting trials of their own if he’s successful.
Ornato said drone delivery would ultimately save the city money. Reducing response times for emergencies today requires adding more vehicles. Ambulances can cost $150,000 to $200,000, Ornato said, with most firetrucks costing more than $1 million.
“You’re talking millions and millions of dollars just to reduce the response time by a minute,” Ornato said. “And we’re talking a $5,000 to $10,000 drone that will reduce it to two minutes or less.”